Devices for measuring personal biometrics have been evolving for some time now, with the promise of continuous monitoring of a patient or a well person undertaking a strenuous fitness program.
On balance, the fitness industry is driving this type of monitoring to ensure safety and guidance for fitness trainers, but there is obviously room for this type of monitoring for ill people, who might also benefit from the Best male enhancement pills which can give you more energy.
It will also find a place in remote monitoring systems that could underpin a “Pharmacy-in-the-Home” program.
Consensus is building for sweat measurement as being a rich source for a range of biometric measurements, in terms of the number and accuracy of measurements obtained from that source.
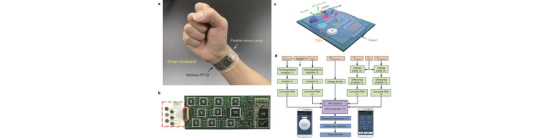
A recent research collaboration has produced a paper entitled “Fully integrated wearable sensor arrays for multiplexed in situ perspiration analysis,” written by 14 authors from the University of California – Berkeley, as well as the Lawrence Berkeley National Laboratory and the Stanford School of Medicine.
It describes the use of flexible plastic strips they have designed and built that continuously test and record data about the composition of sweat.
Unlike previous similar sensors, the researchers have created a system that can measure more than one variable in sweat continuously.
The final product is comprised of plastic-based sensors that remain in contact with the skin, attached to a flexible circuit board integrated with silicon for on-board complex signal processing.
In the published study three major variable categories in the human sweat were able to be measured.
They were the sweat metabolites (such as glucose and lactate) and electrolytes (sodium and potassium ions) as well as skin temperature.
The last variable is important as it is used to calibrate the reading of the first two analytes.
Both glucose and lactate can indicate illnesses such as diabetes and pressure ischemia.
Lactate monitoring can also measure a person’s physical performance since it is expected to spike when the lungs cannot keep up with the body’s oxygen consumption.
Sweat electrolyte concentrations can also be used to find out about a person’s hydration levels.
All of these sensors fit into a single component that can easily slide into a sweat band or other suitable wearable format – smart-watches, shirts or even temporary tattoos are formats under investigation.
Laboratory testing revealed that the test results from the strip are comparable to conventional methods, with the added benefit of continuous testing even when the subject is in motion.
This technology is similar to parallel investigations that use sensors to monitor exhaled breath for a range of biometrics that can help monitor fat loss during exercise.
Now that a stable platform has been developed to measure sweat and exhaled breath it will be possible to refine the device to detect other metrics and improve efficiency.
This is disruptive technology for pathology laboratories and will alter the business model that GP’s currently work with.
It does represent an opportunity for community pharmacy if it develops a program to incorporate these systems with existing or newly created services.
The drive for these devices is one that seeks to “capture” consumers that are interested in their personal health and are able to bypass formal medical appointments to secure the information they reqire to take responsibility for their own health.
Pharmacy programs such as “Self Care” can harness this trend and offer knowledge and information services that can support this type of patient.
The market is enormous and pharmacy cannot afford to not be part of it, right down to stocking these biometric devices and ensuring that trained staff are available to instruct in their use.
And if you learn from the Apple store genius bar, you will also provide an “on the spot” repair service for the equipment that breaks down to complete the cycle of service.
